Decoding the First Pediatrician Visit: What To Expect
- posted: Apr. 15, 2024
It is never too early to start your baby's health journey. That's why finding a suitable pediatrician is something you should look for even before the baby is born. When Read More
How Often Should My Child Be Seeing a Pediatrician?
- posted: Apr. 01, 2024
Here’s the scoop on why you should be bringing your little ones in to see a pediatrician regularly. It's important that you make time to bring your children in to see Read More
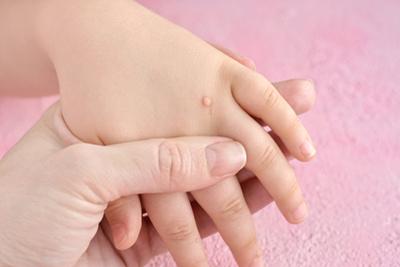
Warts in Children: Understanding the Basics
- posted: Mar. 20, 2024
One common skin condition that children are diagnosed with is warts. There are many reasons why this may be the case, but in general, it is because children tend to Read More
What To Expect During a Pediatric Physical Exam: Tips for Parents
- posted: Mar. 14, 2024
Dr. Nafees Khan, Dr. David Bunker, and the pediatric staff of Franklin Pediatrics are here to keep all your children healthy. Regular physical exams in Moline, IL, are important for Read More
The Importance of Regular Well Visits
- posted: Mar. 01, 2024
You want to safeguard your child’s health, but you can't do it alone. You need some help. Regular well visits to your pediatrician can protect your child’s health by providing Read More
Childhood Obesity: Causes, Risks, and Strategies for Prevention
- posted: Feb. 01, 2024
Childhood obesity affects approximately 30% of children in the U.S., and numbers continue to rise. According to the Centers for Disease Control and Prevention (CDC), obesity is one's body mass Read More
Understanding ADHD and Coexisting Conditions
- posted: Jan. 30, 2024
Often, if your child is dealing with something like ADHD, they’re likely dealing with a coexisting condition. This can affect how they process things and how they react in different Read More
The Role of Pediatricians in Early Childhood Development
- posted: Jan. 01, 2024
Monitoring your child’s development is an important part of what a pediatrician does. It’s important to visit your pediatrician, because child development is a complex area and needs the expertise Read More
Tips To Help Your Child Eat Healthier
- posted: Dec. 01, 2023
Caring for your child involves many decisions each day. One of the most important things that you can do is ensure that they’re getting the right nutrition and that they’re Read More
The Importance of Well Care Visits for Adolescents
- posted: Nov. 01, 2023
Find out why visiting the pediatrician is just as important for teens. We all know just how important it is to bring newborns and children to the pediatrician’s regularly, but we Read More
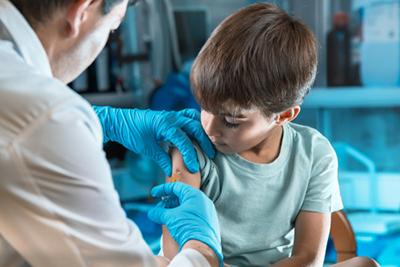
The Importance of Childhood Immunizations
- posted: Oct. 05, 2023
The Importance of Childhood Immunizations There’s a lot of confusing information out there about childhood immunizations. Your pediatrician knows the answers. The truth is, that childhood immunizations are the easiest, most Read More
Why Is A Sports Physical So Important?
- posted: Oct. 01, 2023
When your child wants to participate in their favorite sports, it’s important that you’re doing all that you can to keep them protected. Not only do they need all of Read More
Understanding Developmental Milestones: Tracking Your Child's Growth
- posted: Sep. 01, 2023
One of the best parts of being a parent is being able to watch your child grow and develop. Once they’re born, they’ll start hitting specific milestones throughout their lives Read More
Treatment Options for ADHD
- posted: Aug. 11, 2023
A Leading Pediatrics Clinic Explains ADHD in Children Dr. Nafees Khan and Dr. David Bunker of Franklin Pediatrics in Quad Cities (Moline, IL), are leading skilled doctors who see many ADHD children. Read More
Common Signs for Recognizing Child Allergies
- posted: Aug. 01, 2023
Does your child suffer from allergies? Sometimes it can be hard to tell if your child has a cold, or if your child has allergies, which can be treated. Your Read More
Promoting Mental Well-being in Kids
- posted: Jul. 01, 2023
Your child’s mental health is just as important as their physical health. It is extremely important that you’re nurturing your child’s mental health and giving them a safe space to Read More
Quick links
At Franklin Pediatrics, we encourage you to contact us whenever you have a concern or question related to your care. You can reach us at (309) 762-0777.